
12,000 Americans will turn 65 each day in 2024. And the percentage of the US population above 65 will continue to grow. It’s no surprise then that health plans’ interest in Medicare Advantage has reached a high.
On February 1, Softheon and the Association of Community Affiliated Plans (ACAP) co-hosted a webinar, “Entering Medicare Advantage as a Regional Health Plan.” Watch the full recording here.
Softheon shares the results of a “Priorities in Medicare Advantage” survey conducted with ACAP members, and Cox HealthPlans shared their experience entering Medicare Advantage. Here are 4 key takeaways from the discussion.
1. Survey Says: It’s Time to Invest in Member Experience and Admin Capabilities
Medicare Advantage plans now cover over 50% of Medicare beneficiaries. There’s still a lot of growth left, but that growth is tempered by important challenges. Kevin Deutsch, Softheon SVP and GM of Health Plan Cloud, shared some of those challenges highlighted in the survey.
When it comes to Member Experience, the survey showed a wide range of technical and business capabilities are needed to drive shopping conversion and member retention.
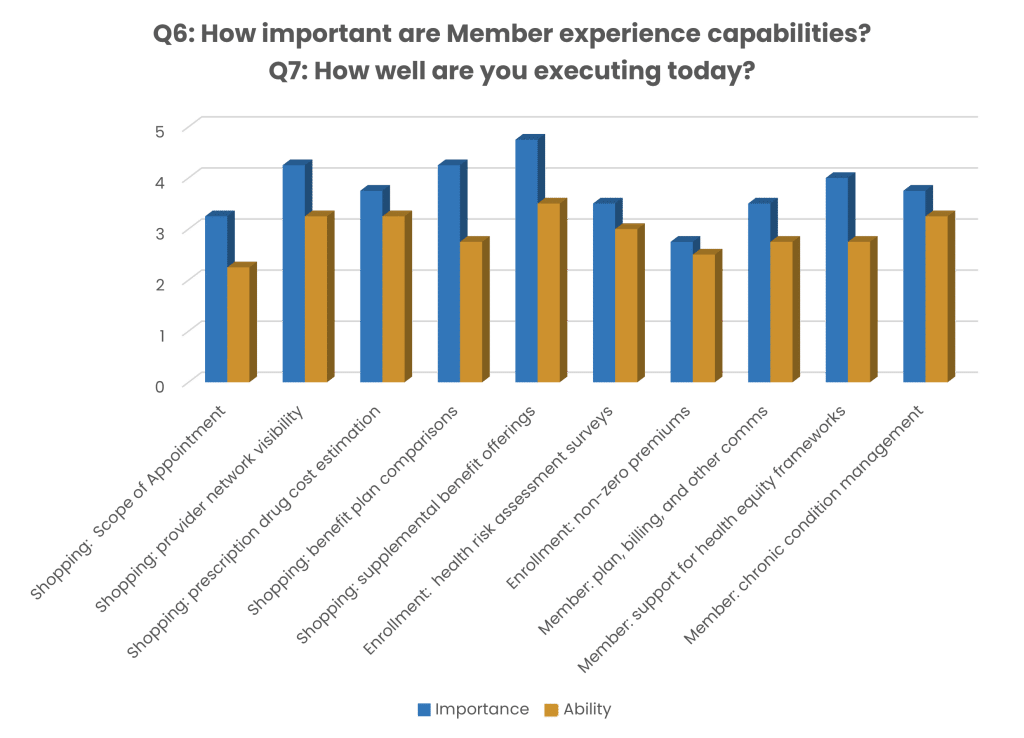
ACAP Plans Survey Results: Member experience capabilities
Top of mind was the ability to create a strong shopping experience, especially for supplemental benefits, provider network visibility, and plan comparison. Health plans indicated they needed to improve execution in all areas, with the most critical capability, supplemental benefits, showing the largest execution gap.
The importance of administrative capabilities ranked highly among ACAP plans, with most capabilities weighted a 4 out of 5.

ACAP Plans Survey Results: Admin capabilities
Health plans rated administration capabilities supporting Social Determinants of Health (SDOH) and member analytics as most important, and where they also had the largest execution gaps. The biggest discrepancy between importance and ability was for AI application. As the only capability with an ability ranking at 1 out of 5, chatbots and other AI applications is an area ready for tremendous growth.
2. Lean on Medicare Advantage Experts to Improve Relationships with CMS
Health plans with experience in the Affordable Care Act (ACA) marketplaces know that it can be a challenge working with the Centers for Medicare and Medicaid Services (CMS). Working with CMS on Medicare side can be even more challenging, with different and shifting rules, policies, and processes.
One example: Star ratings, which measure the quality of Medicare Advantage health and drug services received by consumers. The ratings use 38 different performance measures, and those measures continue to change. Star ratings have a big impact on Medicare Advantage plan profitability. The result? Medicare Advantage health plans need to spend a lot of time and money to stay profitable while providing a mix of high-quality services that support complex member needs.
Other CMS challenges include siloed data, outsourced support centers and outdated technology. To combat this issue, health plans need experienced staff to work across a wide range of design and operational issues.
The Webinar’s guest speaker, Susan Sanchez, CIO of Cox HealthPlans, a community based, provider-sponsored health plan based in southwestern Missouri, shared how challenging the lack of Medicare Advantage expertise is. Critical to their success in entering the Medicare Advantage marketplace was a humility in understanding they needed help to build that operational expertise.
3. Member Experience is the #1 Priority for Cox HealthPlans
Member experience is heavily impacted by Star ratings and the Consumer Assessment of Healthcare Providers and Systems (CAHPS) surveys. And the Over 65 population has unique needs and expectations that are quite different from ACA or private health insurance.
As Anne Taylor, Director of Consulting Services at Softheon, said during the panel discussion, health plans need to find the right balance of all the possible activities that can impact member experience. The key is understanding the gap between what you’re doing today in the member journey vs. where you can have the most impact.
One major component of member experience: brokers. Almost all Medicare beneficiaries use brokers to select a Medicare Advantage plan. Susan from Cox HealthPlans said that their investment in the broker community, including education and customized communications, was critical to getting brokers excited. That excitement in turn is needed to excite beneficiaries to become plan members.
When Kevin asked Susan what Cox HealthPlans’ #1 thing a regional or community plan should prioritize when entering Medicare Advantage, it came right back to member experience: have a strong intake, grievance, and appeal department. This community wants and needs to be heard, and the health plan is often their first line of help in an often confusing and complex health care landscape.
4. Find the Right Partners that can Simplify Operation
Finding the right technology partners is critical to help make sense of member needs data from surveys and engagement touch points, and to give plans the insights they need to confidently improve plan design and execution.
Rasesh Joshi, Principal Medicare Cloud Solution Architect at Softheon, noted during the panel discussion that health plans need to balance technical perspective with the processes they support. Health plans need a partner that has experience capturing CMS processes, audit requirements and other nuances, and build it into their solutions. Partners can also help manage what is automated vs. what is handled manually, as these can directly impact on member engagement and abrasion.
In the discussion, Cox HealthPlans also credited their successful entry with multiple partnerships that helped with technology, back-end processes such as risk adjustment, and member experience such as augmented customer service hours, dental coverage, and rewards and fitness programs.
Medicare Advantage: Ready to Jump In?
As an ACAP Preferred Vendor, Softheon can be your Medicare Advantage “phone a friend” lifeline. Build off your existing ACA experiences and lean on our technical and market expertise to help you decide when you’re ready to jump into the growing Medicare Advantage market.


